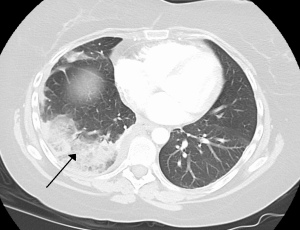
 In March of 2026 I had the terrifying experience of having a Pulmonary Embolism. Two actually, accompanied by two infarcts (lung tissue death) with one in each lung. Oh, and a pleural effusion for good measure. I was transferred (almost airlifted) to a Level II trauma center where I spent two days in the ICU and two more in a regular room. It was a rough few days.
In March of 2026 I had the terrifying experience of having a Pulmonary Embolism. Two actually, accompanied by two infarcts (lung tissue death) with one in each lung. Oh, and a pleural effusion for good measure. I was transferred (almost airlifted) to a Level II trauma center where I spent two days in the ICU and two more in a regular room. It was a rough few days.
Here’s how it all unfolded.
History: At the time of this event I was a 61 year old male living in NJ with a history of lower back pain, right foot problems, a former kidney stone, an appendectomy, and various other joint-related problems and surgeries due to a decade of abusing my body with martial arts in my 20s and 30s.
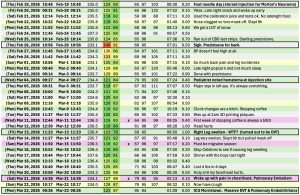
As a quick aside, it may seem odd how detailed my notes are, but due to a blood pressure scare about two years earlier, I take my vitals every morning and record them into an Excel spreadsheet. My primary care provider loves me. [1]
 January 1: We had a huge snowstorm and we had to use the Generator, which is manual, on wheels, and very heavy.
January 1: We had a huge snowstorm and we had to use the Generator, which is manual, on wheels, and very heavy.
I hurt my back moving it because my brain constantly insists that I’m 18 at the most while my spine was screaming that it’s been over 40 years since I was 18.
Oh, and by very heavy I mean 231 pounds which is weirdly almost exactly how much I weighed at the time.
 January 5th: A mere four days later my back felt better so I decided to move one of my gorgeous expensive telescopes. Good telescopes and their trappings are heavy. Hell, it’s got weights to make it even heavier! Why’s it on the second floor? That’s complicated, but if you’re curious it’s a Takahashi TSA-120 on a Tenma 2 EM-200 mount with a gorgeous wooden tripod and it is ludicrously heavy. I had removed the scope and then proceeded to remove the counterweights and then took the mount off the tripod forgetting once again that I am not 18. The mount weighs about 36 pounds, but being as high as it is on the tripod, well…
January 5th: A mere four days later my back felt better so I decided to move one of my gorgeous expensive telescopes. Good telescopes and their trappings are heavy. Hell, it’s got weights to make it even heavier! Why’s it on the second floor? That’s complicated, but if you’re curious it’s a Takahashi TSA-120 on a Tenma 2 EM-200 mount with a gorgeous wooden tripod and it is ludicrously heavy. I had removed the scope and then proceeded to remove the counterweights and then took the mount off the tripod forgetting once again that I am not 18. The mount weighs about 36 pounds, but being as high as it is on the tripod, well…
It felt like someone stuck a knife wired to a cattle prod directly into my spine.
January 8: Had an appointment with an Orthopedic Physician’s Assistant (Ortho PA) since the surgeons were all booked for months. My wife, Lauren, had to drive me to this appointment because I was in so much pain. The Ortho PA said my symptoms were indicative of a ruptured disc between L5 and S1 and she wanted me to do physical therapy (PT) but I resisted because could barely move myself around let alone get to PT and exersize.
February 12: Got an MRI of my right foot to identify the location of a Morton’s Neuroma for potential steroid injection. This foot problem had been going on for years and we had already done one or two injections (I forget). I’m old – what can I tell you?
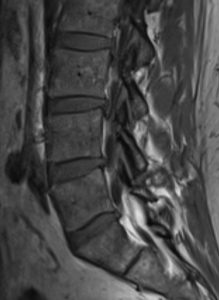 February 17: Got an MRI of my lower back after complaining to the Ortho PA that nothing was being done for my back pain given that my foot had been numb for over a month after my back injury in January. I had forced the issue by offering to pay for the MRI since insurance was resistant to do so since I had not done any PT.
February 17: Got an MRI of my lower back after complaining to the Ortho PA that nothing was being done for my back pain given that my foot had been numb for over a month after my back injury in January. I had forced the issue by offering to pay for the MRI since insurance was resistant to do so since I had not done any PT.
February 19: Got a steroid injection from my podiatrist in my right foot to help with the previously mentioned Morton’s Neuroma. This was the second or third injection in this foot over the span of probably 18-24 months. The injection hurt more than the previous injections, but needles hurt, so I didn’t think anything of it.
February 26: The Ortho PA was on vacation for a week so I finally got my MRI results which indeed showed a ruptured disc between L5 and S1 in my lower back so she started me on a 7-day course of Prednisone. My blood pressure (which I track daily) went from a nominal 122/80 to 140/91 and stayed elevated for the days I was on Prednisone. The Ortho PA told me again to go to PT which I, again, did not.
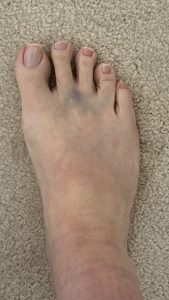 March 4: At my follow-up with the podiatrist I told him that my foot was still bruised he said something to the effect of, Sorry for the hematoma (bruise) – may have nicked a vein. It did not hurt, but it looked ugly, and since it seemed like a minor thing none of us were concerned. He couldn’t really do anything for my foot with my back interfering and so now I was at the point with competing doctors who weren’t talking with each other due to being affiliated with different hospitals.
March 4: At my follow-up with the podiatrist I told him that my foot was still bruised he said something to the effect of, Sorry for the hematoma (bruise) – may have nicked a vein. It did not hurt, but it looked ugly, and since it seemed like a minor thing none of us were concerned. He couldn’t really do anything for my foot with my back interfering and so now I was at the point with competing doctors who weren’t talking with each other due to being affiliated with different hospitals.
For the record, I love the podiatrist – the Ortho PA, not so much.
For the next nine or so days everything seemed back to normal except for a stye in my left eye which has nothing to do with this story but I would like to state for the record that I did not enjoy it and given the choice would not have one again.
March 11: I noted in my log that I had a migraine, but I get enough headaches (and always have) that I log them. I would proceed to have three migraines in the span of 11 days which is very unusual for me since I usually get maybe one every 3-4 months. Migraines are vascular in nature, so this was a possible sign that something was up.
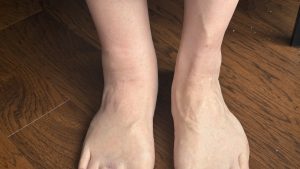 March 13: While taking a shower I noticed that one leg was very swollen. In my daily vitals log I wrote, Right leg swollen, WTF? It did not hurt, it was not red, and it was not hot, but I had been dealing back pain with all sorts of right leg symptoms, so this just seemed like another one. Why do I have all these pics? Because I am an obsessive data hoarder who was an engineer and consultant for decades. Any time anything unusual happens to me (or around me) I take pictures because they help me determine a root cause later, if need be.
March 13: While taking a shower I noticed that one leg was very swollen. In my daily vitals log I wrote, Right leg swollen, WTF? It did not hurt, it was not red, and it was not hot, but I had been dealing back pain with all sorts of right leg symptoms, so this just seemed like another one. Why do I have all these pics? Because I am an obsessive data hoarder who was an engineer and consultant for decades. Any time anything unusual happens to me (or around me) I take pictures because they help me determine a root cause later, if need be.
In retrospect, this was I should have gone to the ER moment #1.
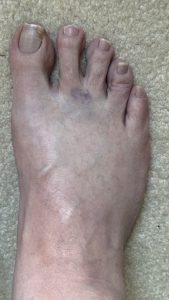 March 14: I took this picture of my swollen foot because I thought it was interesting that I still had the bruise from the injection which I had received just shy of a month prior (February 19). Note the swelling in my foot compared to the previous picture. That is not a happy foot.
March 14: I took this picture of my swollen foot because I thought it was interesting that I still had the bruise from the injection which I had received just shy of a month prior (February 19). Note the swelling in my foot compared to the previous picture. That is not a happy foot.
March 16: I had been taking a bunch of Celebrex for my back and suspected that may have been the cause since swelling of the hands and feet is listed as a common side effect. I stopped taking it on this day and lost one pound per day for the next few days. I presumed this to be fluid loss from the swelling going down and therefore I assumed the Celebrex to be the culprit, thundering hooves generally not being zebras, and all that.
March 17: I Drove to PA from NJ to have dinner with friends on the 17th. I spent most of the night with my foot up on the chair opposite me at the table because my leg was bothering me. Dinner was great.
March 19 (Thursday): I had a follow up with my Ortho PA to discuss my spine and showed her my leg. There seemed to be no sense of alarm about me having one swollen leg, but stopping the Celebrex had helped diminish the swelling, so I imagine me telling her that biased her opinion of me having a swollen leg.
After leaving the Ortho office I started to feel awful in the I have a fever malaise sort of way, and managed to get an appointment with my primary’s office, though not with my primary but rather a new Nurse Practitioner who I had never met. I showed him my leg, and he did not seem to be alarmed, though I can’t dismiss the possibility that I sort of biased both healthcare workers’ differential diagnoses by telling them that I thought it was the Celebrex. I assumed I had a sinus infection because I have a history of them, and he gave me a blood test and sent me home.
March 20 (Friday): I woke up feeling even worse so I called my primary’s office and said I wanted antibiotics because I’m very familiar with how an infection feels, and I was sure that I had one. They scheduled me for an afternoon visit, then called me back a short while later. One contentious phone call later (followed up by a nicer call with someone else) I got antibiotics phoned into my pharmacy and they cancelled my appointment.
When we picked up the antibiotics that evening I discovered that they were Doxycycline (Doxy). I dislike Doxycycline because I had a bad experience with it in my 20s in which I wasn’t warned to take it with food. Not completely swallowing the Doxy managed to cause an ulceration in my esophagus which woke me up in the early morning thinking I was having a heart attack. Had I known that’s what he was giving me this time I would have insisted on something else, but by this point it was late Friday and the offices and pharmacy were closed so I carefully took the meds two full hours before bed with both food and a large amount of water. Having had a kidney stone years prior I also habitually drink a lot of water.
March 21 (Saturday): I woke up at 2am with chest pain. Given my history with Doxycycline I assumed that’s what this was. The doctor’s office is closed on Saturday, so I called the on-call, which was a disaster through no fault of the service or the office. My phone blocks unknown numbers so all the callbacks went to voicemail, and all the voice mails were just “we’ll call you back” with no number shown and no way for me to call them back directly. My primary was the on-call, so it kind of sucks that I didn’t get to talk to her because she would have sent me to the ER right away.
This was I should have gone to the ER moment #2.
March 22 (Sunday): I was not able to sleep because it hurt to breathe. Laying flat I had a pain in the middle of my chest that felt like Doxycycline had burned a whole in my esophagus while laying on either side felt like there was a knife stuck between my ribs on the side facing down. I managed to get a couple hours of fitful sleep in the recliner, but at this point I assumed it was something like pneumonia which would have explained the feverish feeling and the pains. Of course it was something far worse. I had also started having an annoying dry cough.
This was I should have gone to the ER moment #3.
 March 23 (Monday): One of the first signs that clicked for me that something was seriously wrong was when I walked back from the bathroom near my home office at 8am. This is a distance of about 10 steps and I was severely out of breath, so I took my PulseOx which measured 112/82. I then quickly grabbed my phone and captured this pic of it at 101/85. I was recovering quickly, but any Sp02 (blood oxygen saturation) below 90 is cause for alarm.
March 23 (Monday): One of the first signs that clicked for me that something was seriously wrong was when I walked back from the bathroom near my home office at 8am. This is a distance of about 10 steps and I was severely out of breath, so I took my PulseOx which measured 112/82. I then quickly grabbed my phone and captured this pic of it at 101/85. I was recovering quickly, but any Sp02 (blood oxygen saturation) below 90 is cause for alarm.
I was lucky I didn’t pass out.
This was I should have gone to the ER moment #4.
Since I was up so early (uncommon for me) I could call my primary’s office when they opened at 9am and explained what was going on. The front desk talked to my primary who said simply, “Go to the hospital.”
I was not in distress. Sure it hurt to breathe deeply and my annoying dry cough now hurt a bit, and it hurt to lie down, and sure my Sp02 had dipped into the “pass out” territory more than once, but I otherwise felt fine. As such, I told my wife to go take a shower and I would make myself breakfast, which I did.
This was I should have gone to the ER/I am an Idiot Moment #5[2]
After breakfast we took a leisurely drive to Hackettstown Medical Center. We discussed going to Morristown Medical Center (a Level II Trauma center and all around better hospital that is farther away) but we both assumed that I had pneumonia and they would just give me antibiotics. I cannot convincingly convey how neither of us thought anything serious was going on. We are both smart people and my wife has watched all the doctor shows yet neither of us put the clues together.
 My wife dropped me off at the ER so she could park and I walked in on my own. I said to the receptionist that it hurt to breathe so they got me into a wheelchair, took my info, then as soon as my wife came in they let her do the paperwork while they rolled me into triage where they did triage things. They then rolled me into a room in the ER. I even took pics to send my kids (both in their 20s and living in Brooklyn). We told them I was fine and not to worry because it was probably just pneumonia.
My wife dropped me off at the ER so she could park and I walked in on my own. I said to the receptionist that it hurt to breathe so they got me into a wheelchair, took my info, then as soon as my wife came in they let her do the paperwork while they rolled me into triage where they did triage things. They then rolled me into a room in the ER. I even took pics to send my kids (both in their 20s and living in Brooklyn). We told them I was fine and not to worry because it was probably just pneumonia.
The nurses were fabulous. They asked me all sorts of questions while my wife and I continued assuming that I had pneumonia. They sent me for a chest CT and we waited for results.
After a while a grumpy old doctor came in with an ultrasound machine and scanned my leg and my chest. He then said in his cranky old man voice as if talking to a teen who had been caught drinking, and I quote: “You have massive clots in your right leg and a pulmonary embolism in each lung. Do NOT get out of that bed, even to use the bathroom or you will have THE MOTHER OF ALL HEART ATTACKS. You need to be airlifted to Morristown immediately.” He then rolled his machine out the door and left where the two of us looked at each other wide-eyed and thunderstruck.
What. The. Fuck.[3]
My wife says that was the scariest moment of her life. I never thought about quantifying and sorting my scariest moments before, but I can say with certainty that I had never before been confronted with a statement like “stay in bed or you’ll die”, so yeah, if it’s not #1 on the list for me, it’s up there.
My heart rate damn near doubled. My blood pressure (which I took that morning and recorded as 122/87) was 152/90 and that was after some time when the nurse came in to check. You know what you shouldn’t do to someone you’re worrying about having THE MOTHER OF ALL HEART ATTACKS after dual pulmonary emoboli? Double their heart rate through anxiety, fear, and maybe even panic. It was as if someone said, you should sit still and avoid stress and also <pulls out a gun> STAY CALM OR I’LL SHOOT! It was surreal.
Airlift? Isn’t that for car crashes and gunshot victims? I feel fine. Lauren and I had been joking with each other before Dr. Doom came in. Don’t I just have pneumonia? My chest hurts. What the hell is happening?
Luckily, a short while later (which felt like 12 hours) the head ER doctor and the wonderful nurse came in to calmly and rationally explain everything to us. I had massive Deep-Vein Thrombosis (DVT) in my right leg, the clots had separated and lodged in each of my lungs (bilateral pulmonary emboli), each of which causing infarction (tissue death). In short, the pain was due to parts of my lungs dying. Neat. <cough> (ow). Oh, I also had Pleural Effusion when means fluid between my lungs and the tissue that surrounds them because I guess the other stuff wasn’t exciting enough for a Monday morning. We made sure to complain about the previous doctor’s utter lack of compassion and bedside manner, a complaint about which they did not seem surprised.
My wife texted the kids to come home right now and to meet us at the hospital in Morristown. I can’t imagine how scary reading that text must have been for them.
The nurse then came in and gave me an IV line in each arm along with a couple of blood tests. Two IV lines seemed excessive, but who am I to complain? She said that they would be starting me on blood thinners and that getting two IVs now was easier than adding one after the blood thinners since adding one later would “make me bleed like a stuck pig”. We loved that nurse; she made everything better.
Literally three hours after being told to not even get up to pee or I’d get THE MOTHER OF ALL HEART ATTACKS, we met two very nice paramedics who would be driving me to Morristown because weather had grounded the MedEvac helicopters. I was both disappointed that I wouldn’t get to ride in the helicopter and relieved that I didn’t need to ride in the helicopter (which was not the case). I was told that there would be an ICU room waiting for me and a surgical team on standby in case they needed to go in and remove clots from my heart. Yikes.
 The ride in the ambulance was uneventful and we had a great chat on the way, which was probably them keeping me talking in order to make sure that I was not having THE MOTHER OF ALL HEART ATTACKS in the ambulance. We arrived at Morristown a short while later after needing to move over for a State Trooper with his lights on (we did not have our lights on) and then I got to witness the most amazing ballet of precision and professionalism I think I’ve ever seen.
The ride in the ambulance was uneventful and we had a great chat on the way, which was probably them keeping me talking in order to make sure that I was not having THE MOTHER OF ALL HEART ATTACKS in the ambulance. We arrived at Morristown a short while later after needing to move over for a State Trooper with his lights on (we did not have our lights on) and then I got to witness the most amazing ballet of precision and professionalism I think I’ve ever seen.
 They rolled me directly into the Medical Intensive Care Unit (ICU) where a nurse was standing in the back of the central hub holding up six fingers, which meant I was going into room six. They rolled me up next to the bed, were thrilled that I could scooch myself over, and then the paramedics left. I then had probably six nurses descend on me who managed to do the following while I tried to keep up: Undress me, give me a sort of super-quick sponge bath, put a gown on me, wire me up to the EKG, hook me up to a new Heparin drip, hook me up to oxygen, take my temperature, ask me who I was, what my birthday was, if I knew where I was, why I was there, what day it was, what month it was, and what the date was (I failed this one, LOL), put all my stuff in a bag and then the swarm left and I was left with one nurse. I felt like a Formula One car that just had a pit stop.
They rolled me directly into the Medical Intensive Care Unit (ICU) where a nurse was standing in the back of the central hub holding up six fingers, which meant I was going into room six. They rolled me up next to the bed, were thrilled that I could scooch myself over, and then the paramedics left. I then had probably six nurses descend on me who managed to do the following while I tried to keep up: Undress me, give me a sort of super-quick sponge bath, put a gown on me, wire me up to the EKG, hook me up to a new Heparin drip, hook me up to oxygen, take my temperature, ask me who I was, what my birthday was, if I knew where I was, why I was there, what day it was, what month it was, and what the date was (I failed this one, LOL), put all my stuff in a bag and then the swarm left and I was left with one nurse. I felt like a Formula One car that just had a pit stop.
I was assigned the status NPO (from the Latin nil per os) which means nothing by mouth – not even water except for sips necessary to take pills. This was in case I needed emergency surgery and was sort of an enforced “no food after midnight” thing (think surgery, not Gremlins). Thanks to the stress about possibly having THE MOTHER OF ALL HEART ATTACKS my appetite was nonexistent, so this rule was surprisingly easy for me to follow.
 My kids (Meghan and Colleen) arrived before any of us because the helicopter was cancelled and I had to wait three hours, so even with them traveling from NYC and taking an Uber from the train station they arrived at the ICU before us and had to wait in the Family Waiting Area until I arrived. Meghan took this selfie pic which I only saw a month later and it’s easily become my favorite of them all. When I asked her why she took it she replied, “Because I thought it would be funny and I was so stressed out and happy that you weren’t going to die.”
My kids (Meghan and Colleen) arrived before any of us because the helicopter was cancelled and I had to wait three hours, so even with them traveling from NYC and taking an Uber from the train station they arrived at the ICU before us and had to wait in the Family Waiting Area until I arrived. Meghan took this selfie pic which I only saw a month later and it’s easily become my favorite of them all. When I asked her why she took it she replied, “Because I thought it would be funny and I was so stressed out and happy that you weren’t going to die.”
My wife (Lauren) arrived and we tried to diffuse the stress with humor as best we could with the threat of THE MOTHER OF ALL HEART ATTACKS and emergency surgery ever hanging over us. When dinnertime came and went I sent them home to get some rest because as much as I loved them being there, I was where I needed to be and they needed to get some sleep.
Every four hours I had to have a blood test to check my clotting numbers, and that meant that I could not sleep for more than about three hours and fifty minutes. So many needles; I did not get much sleep. Using the submarine toilet was an adventure that at this point I decided that I did not enjoy.
My Heparin IV kept throwing a “downstream occlusion” error every few minutes which would beep loudly enough to wake me up. The nurse would come in, tell me to keep my elbow straight, but no matter what I did it would throw another alarm mere minutes later. This was a great way to further prevent me from sleeping during the brief reprieves between needle jabs.
March 24 (Tuesday): My wife called me at 6:30am and when I didn’t answer she naturally assumed that I was dead. Therefore she was in my room by 8am after what surely must have been a stressful drive after an exhausting night on top of all of the previous day’s stress.
A delightful ultrasound tech came in and re-scanned all my veins, or at least the ones that mattered. I couldn’t see the screen because of the way I needed to be oriented, but my wife said that it looked like there were marbles in my veins. Big crusty death-dealing clot marbles.
At some point one of the nurses brought in a device for me to use that I quickly nicknamed The Infernal Machine.
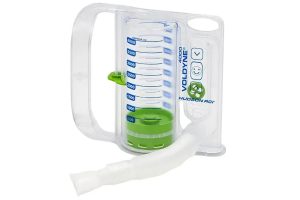 The Infernal Machine is actually called an Incentive Spirometer and it’s used to exercise your lungs in a way that someone with recent pulmonary emboli might find positively diabolical. Basically you suck on the tube and aim to raise the green puck in the cylinder up to the marked capacity. She handed it to me and said, “use this 10 times every hour and try to get to 1500ml.” I took it, got there with ease, and figured that was that. She said, “Oh, good!” and then raised it to 2500ml and suddenly my favorite nurse was my nemesis. You see, expanding my lungs by filling them with air hurt and made me cough like crazy. Why would anyone submit a pulmonary embolism patient to the infernal machine? Because it works.
The Infernal Machine is actually called an Incentive Spirometer and it’s used to exercise your lungs in a way that someone with recent pulmonary emboli might find positively diabolical. Basically you suck on the tube and aim to raise the green puck in the cylinder up to the marked capacity. She handed it to me and said, “use this 10 times every hour and try to get to 1500ml.” I took it, got there with ease, and figured that was that. She said, “Oh, good!” and then raised it to 2500ml and suddenly my favorite nurse was my nemesis. You see, expanding my lungs by filling them with air hurt and made me cough like crazy. Why would anyone submit a pulmonary embolism patient to the infernal machine? Because it works.
 My daughters Colleen and Meghan came in at some point having enjoyed a morning of sleep (probably) unmarred by fear of my demise. Colleen brought me a wonderful gift, which was Nigel the Little Elephant. Years prior when Colleen had been in this same hospital for an emergency appendectomy, I had bought this little metal elephant in the gift shop because I thought it was something she would love. When she got home she clutched it tightly and when her friends visited and asked how she was doing, she would whisper in her drugged fugue, “I have a tiny elephant”. It was adorable, and I later put it into a little jar for safekeeping so it would be more difficult to lose. Nigel the tiny elephant stayed close to me on my portable bedside table and he made everything better. He even made the four-hour needle visits seem almost tolerable. Almost.
My daughters Colleen and Meghan came in at some point having enjoyed a morning of sleep (probably) unmarred by fear of my demise. Colleen brought me a wonderful gift, which was Nigel the Little Elephant. Years prior when Colleen had been in this same hospital for an emergency appendectomy, I had bought this little metal elephant in the gift shop because I thought it was something she would love. When she got home she clutched it tightly and when her friends visited and asked how she was doing, she would whisper in her drugged fugue, “I have a tiny elephant”. It was adorable, and I later put it into a little jar for safekeeping so it would be more difficult to lose. Nigel the tiny elephant stayed close to me on my portable bedside table and he made everything better. He even made the four-hour needle visits seem almost tolerable. Almost.
At 11:30am I got a Transthoracic Echocardiography which means they did an echo of my heart. Meghan watched from the corner, fascinated to compare my heart to hers since she has had scans of her own. Hey – family time is family time!
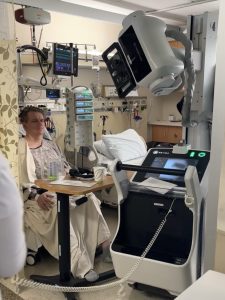 Later, the nurses (I assume) decided that it would be good for me to sit in the chair, so they got me moved after which various doctors and nurses came in asking me all sorts of medical things. They rolled a portable X-Ray machine into my room, ushered everyone out, yelled “X-RAY” and took a chest x-ray. Picture of me getting a chest x-ray courtesy of my daughter, Colleen.
Later, the nurses (I assume) decided that it would be good for me to sit in the chair, so they got me moved after which various doctors and nurses came in asking me all sorts of medical things. They rolled a portable X-Ray machine into my room, ushered everyone out, yelled “X-RAY” and took a chest x-ray. Picture of me getting a chest x-ray courtesy of my daughter, Colleen.
After a couple of hours, the hematology team came in with the CT scan and ultrasound results and informed me that the clot-load on my heart was zero so there was no need to keep the surgical team on standby and that they would move me into a regular room as soon as possible. That seemed like good news, but I was so overwhelmed with data and experiences and worry that I don’t remember being relieved. I still hadn’t processed any of that and while I don’t remember being relieved, I do remember the nurse coming in and saying, “here’s the menu – you can order lunch.”
“What can I order?”
“You have no restrictions.”
In the span of five minutes I went from worrying about THE MOTHER OF ALL HEART ATTACKS with a crack surgical team on standby and thus not being able to drink or eat anything to being able to order whatever I wanted from the menu. That kind of tectonic shift in reality was as tough to process as the don’t move or you’ll die treatise that started this journey. I said I wanted my wife’s patty melts because she makes the best damn patty melts anywhere, but I think I ordered something boring like a chicken Caesar salad and a ginger ale because if there’s one thing every hospital seems to have in abundance, it’s ginger ale.
With the emergency in the past, root cause analysis became the order of the day and every single doctor and nurse asked the same questions:
- Have you recently flown? Nope
- Any long car rides? Nope
- Have you recently had surgery? Nope
- Do you have a history of heart problems? Nope – High BP was resolved by CPAP
- Do you smoke? Nope
- Are you dehydrated? Nope – had a kidney stone and I drink water constantly
- Family history of DVT? Nope
- How’s your diet? Could be better, but we have real food for dinner every night with a salad most days
- Are you sedentary? I told them I sit all day but get up every hour and go up and down a flight of stairs 10+ times a day to which they said, “there are people far more sedentary than you who don’t get DVTs” so that did not seem to be a concern.
With a lack of a clear cause they considered me idiopathic which means I formed a leg full of clots spontaneously and without cause. In the case of DVT that’s bad because without a root cause I’d need to be on blood thinners for the rest of my life. Yuck.
A wonderful physical therapist came in and had me get up and walk around the ICU which was the first time I got to see the other patients. This was the first inkling I had of just how serious my condition was because they all looked to be on death’s door with endless machines and monitors hooked up to them. I managed to walk up and down the ICU twice trailing my oxygen and IVs which made the therapist happy so after that I got to rest for a bit.
At this point I was consuming an ICU bed that I didn’t require, but there was a backlog of regular rooms so I tried my best to enjoy my large private ICU room with the awesome nurses, lack of privacy, weird submarine toilet, and four-hour needle jabs. Lauren, Meghan, and Colleen made it better every moment they were there. Nigel the tiny elephant made it all bearable during the dark hours when my only other friend was the clock.
At midnight they moved me to a regular room after giving me a sort of one minute sponge bath that I have no doubt I sorely needed. I also had to help the poor girl who moved me because she took a wrong turn in the dark hospital hallways at midnight and I had to help guide her back to where we were supposed to be. My excellent sense of direction and propensity for telling people they’re doing it wrong was apparently unimpaired.
 March 25 (Wednesday): I got to order whatever I wanted for breakfast and got a delicious omelette with American cheese and onions. It was seriously pretty great, so kudos to whoever made it.
March 25 (Wednesday): I got to order whatever I wanted for breakfast and got a delicious omelette with American cheese and onions. It was seriously pretty great, so kudos to whoever made it.
The only soda I really drink is Mexican Coke in the glass bottles (which is difficult to find and thus limits my soda intake), and my daughter Colleen smuggled one in for me. An ice cold Mexican Coke makes even a non-private room in the hospital a better place. Yum.
My temperature kept creeping up and at one point got to 101.5, a fact that the doctors found concerning enough that they wouldn’t let me go home until it was normal (or at least under 100) for 24 hours. They gave me every test they could think of (yay needles!) and they all came up negative. They gave me an IV bag of Zosyn antibiotics to see if that helped because you can never have too many IVs.
 For some reason every time the nurses or even the cafeteria brought me soda, it was diet ginger ale. I’ve always joked with my wife that I don’t drink ginger ale at home because it reminds me of being in the hospital, but while I’m in the hospital it’s great. The problem is that I’m allergic to aspartame (NutraSweet) so I don’t drink diet sodas. As the nurse came in and cleaned up my bedside rolling table she left the diet ginger ale and I commented offhandedly that I can’t drink that. She came back an hour later and told me that it clicked for her that my chart said I was allergic to aspartame and that’s why I said I couldn’t drink the diet soda, so she actually went and hunted down regular ginger ale for me! Every nurse I had was fabulous, but she may have been my favorite.
For some reason every time the nurses or even the cafeteria brought me soda, it was diet ginger ale. I’ve always joked with my wife that I don’t drink ginger ale at home because it reminds me of being in the hospital, but while I’m in the hospital it’s great. The problem is that I’m allergic to aspartame (NutraSweet) so I don’t drink diet sodas. As the nurse came in and cleaned up my bedside rolling table she left the diet ginger ale and I commented offhandedly that I can’t drink that. She came back an hour later and told me that it clicked for her that my chart said I was allergic to aspartame and that’s why I said I couldn’t drink the diet soda, so she actually went and hunted down regular ginger ale for me! Every nurse I had was fabulous, but she may have been my favorite.
I was finally taken off the Heparin drip when my clotting numbers looked right, and with the antibiotics done the freedom from the IV bag was glorious. Oral blood thinners were now good enough it seems. Well, a double-dose of oral blood thinners, anyway.
 They also removed me from the cardiac monitors which seemed like a good thing. I was starting to feel less like a pod-person in The Matrix and more like… someone in The Matrix who has not awakened to the fact that they were in a pod.
They also removed me from the cardiac monitors which seemed like a good thing. I was starting to feel less like a pod-person in The Matrix and more like… someone in The Matrix who has not awakened to the fact that they were in a pod.
In the new room they wanted me to stop using the oxygen, which I wasn’t happy about, but I quickly learned that I really only needed it when I went to the bathroom. Something about sitting upright made me cough like crazy so they showed me how to set the rolling O2 bottle and I was good from then on. Progress!
The physical therapy guy came by with a walker and asked if I’d like to go for a walk. I said, “sure, so long as I don’t have to use that thing.” We walked all the way up and down the hall and up to the landing on the stairs and he seemed pleased, especially since I wasn’t allowed to bring my beloved oxygen tank.
When I got back into the bed the blood pressure cuff was either too loose or not on quite right, so when it inflated automatically it squeezed the IV line in the crook of my right elbow. Not only that, but the computer didn’t like the result and so deflated and inflated the cuff over and over, squashing the IV line again and again until I ripped the blood pressure cuff off my arm. When the nurse came in to see why the computer was unhappy and I told her what happened, she gave me a third IV line lower on my right arm. You really can’t have too many IV lines.
Since I was now free to use the bathroom on my own, at around 11am I went to do so. Since I was no longer hooked up to the portable cardiac monitor the pocket on the front of my gown was available, so I cleverly put my phone and glasses in said pocket while attending to business. Upon standing, I discovered that the pocket is designed not for the patient’s convenience, but rather specifically for holding the cardiac monitor transceiver. I now know this because the pocket has a huge gap in it for the wires connecting the skin probes to the transceiver and that gap is where my phone and glasses ended up.
Put simply, my glasses and phone fell into the toilet.
I quickly (well, as quickly as someone in my condition can be) fished my phone out of the toilet and snapped a pic I have not loaded here. The nurse happened to be there when I opened the door, and to her credit she immediately grabbed my phone and glasses and wiped them down with the antiseptic wipes available pretty much everywhere in the hospital. My wife had arrived when I was in the bathroom and the nurse (who we all loved) said to my wife, “did you hear what he did?” As usual, a good laugh at my expense made everyone feel better.
 I had another portable x-ray taken and the results of this one included my favorite result of all the tests which was, Bones: Grossly intact. Hey, at least I’ve that going for me!
I had another portable x-ray taken and the results of this one included my favorite result of all the tests which was, Bones: Grossly intact. Hey, at least I’ve that going for me!
When I didn’t order lunch the cafeteria picked for me and I got a cheeseless burger that made me laugh just because of how pathetic it looked alone on the plate devoid of not only cheese, but anything else one might add to a burger. My daughter could not pass up a chance to grab a pic of me smiling in the hospital. The crazy part was the fact that the cheeseless burger (you know, a hamburger) was fabulous, and I’ll usually pass on a burger without cheese! Let it be known that the Morristown hospital cafeteria makes some damn good food!
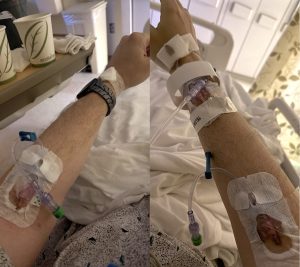 This was the state of my arms at 6:40pm. That’s three IV lines, too many blood draws to count, two ID bracelets (one for ICU and one for the regular room) and some glue the likes of which I might argue has no business being on human skin (or at least human skin that has hair) but I wouldn’t come to that realization until later.
This was the state of my arms at 6:40pm. That’s three IV lines, too many blood draws to count, two ID bracelets (one for ICU and one for the regular room) and some glue the likes of which I might argue has no business being on human skin (or at least human skin that has hair) but I wouldn’t come to that realization until later.
Just before midnight I decided to take another pic of my legs in the hospital bed to complete the set and that’s when I discovered that my phone camera was ruined.
 My kids had started calling my photo updates “feet pics” due to them all being pics of my feet which is funny in a way that I don’t feel like explaining. If you’re too old to get the reference ask your favorite young (but over, let’s say, 15 year-old) person. If you’re too young to get the reference please don’t ask anyone.
My kids had started calling my photo updates “feet pics” due to them all being pics of my feet which is funny in a way that I don’t feel like explaining. If you’re too old to get the reference ask your favorite young (but over, let’s say, 15 year-old) person. If you’re too young to get the reference please don’t ask anyone.
Late at night on the last day of methodical regular needle jabbing, they ordered blood cultures – basically little nips-looking bottles that got my blood added to them to see if whatever nasty was in the bottle would grow. At this point I was really low on places to jab needles, and the poor guy either missed the vein or had to pull the needle out, and blood just flowed down my arm. It was like watching paint with too much thinner in it run down the wall. I know that blood thinners are actually anti-coagulants and don’t actually “thin” the blood, but holy crap did I suddenly understand why everyone calls them blood thinners. I also had a flashback to the nurse in the first hospital’s ER warning me that I would “bleed like a stuck pig”. Ooh… foreshadowing!
I joked with the nurses that I smelled like a pastrami sandwich that someone left on the side of the road a week ago. I assure you, it was worse, and to this day I’m convinced that’s why they eventually let me go.
March 26 (Thursday): I woke up with a mostly normal temperature so they started the process of letting me go home with some prescriptions for Eliquis, Augmentin, and clearance to use regular strength Tylenol as needed. Advil and Celebrex were now off-limits due to being on blood thinners.
The lovely nurse came in and proceeded to pull all of those IV lines out. That wasn’t bad at all, but peeling off the windows around the IVs that were glued to my skin meant pulling the hairs on my arms one by one which I swear was worse than the needles, and at that point I didn’t think there could be anything worse than the needles. She apologized constantly and I felt kind of bad for her even through the drawn-out constant hair-by-hair pain. She was even using the special glue solvent which didn’t do anything so far as I could tell, and she couldn’t just yank them off because they were also taped to the IV lines in my veins.
Once all the paperwork was done they pretty much wanted me gone to free up the bed, and everyone from the guy pushing my wheelchair to the woman running the wheelchair runners was fabulous.
 When I was finally back in Lauren’s car and experiencing the outside again for the first time in the better part of a week, I texted my kids that I was free and they demanded a selfie, the results of which is this foggy urine-soaked phone pic. It was the last pic I took with that phone.
When I was finally back in Lauren’s car and experiencing the outside again for the first time in the better part of a week, I texted my kids that I was free and they demanded a selfie, the results of which is this foggy urine-soaked phone pic. It was the last pic I took with that phone.
My wife asked me what I wanted for dinner. We had her world-famous patty melts and sitting together with my family eating those patty melts may have been the best dinner I’ve ever had.
Finally Home
March 26: I woke Lauren up at 3am. She normally sleeps like a rock but she was instantly awake. I told her that my leg felt funny and I was worried about that so I was going to sit on the recliner with my leg elevated.
She came downstairs and as soon as she walked in I had a complete and utter meltdown. I felt like a toddler sobbing that I don’t want to go back! I don’t want any more needles! It all just exploded out of me and I did not see it coming.
I was a wreck. I had been keeping it all together for so long that I guess it just all had to come out. Being afraid to die can do that to a guy I guess. I can only imagine what they all must have gone through, but for that night at least, Lauren just held me and made everything better.
 March 27: Lauren took this pic of me sitting outside with Sully. I was tired, and my leg hurt, and it was tough to breathe, and… I was home. I have no idea what I was doing on my phone – probably updating friends, but I was home and Sully, our 120 pound Newfoundland dog was there to protect me from anyone who even thought about coming at me with needles. Of course he can easily be bought with hamburgers and he doesn’t care if there’s cheese, but he’s my buddy and he was there with me and I was glad.
March 27: Lauren took this pic of me sitting outside with Sully. I was tired, and my leg hurt, and it was tough to breathe, and… I was home. I have no idea what I was doing on my phone – probably updating friends, but I was home and Sully, our 120 pound Newfoundland dog was there to protect me from anyone who even thought about coming at me with needles. Of course he can easily be bought with hamburgers and he doesn’t care if there’s cheese, but he’s my buddy and he was there with me and I was glad.
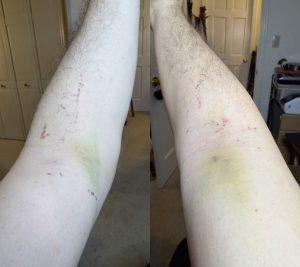 March 28: I took these pictures of my arms a couple days after I got home. I joked that I bet I could get methadone at any clinic just by showing my arms because that’s the kind of dark tasteless humor that sustains me during stressful events. That was about the worst of it, though I had the bruises for almost two weeks thanks to the blood thinners. Well, the blood thinners, a crazed blood pressure computer, and 391 needle jabs. Oh, and one session of glue torture.
March 28: I took these pictures of my arms a couple days after I got home. I joked that I bet I could get methadone at any clinic just by showing my arms because that’s the kind of dark tasteless humor that sustains me during stressful events. That was about the worst of it, though I had the bruises for almost two weeks thanks to the blood thinners. Well, the blood thinners, a crazed blood pressure computer, and 391 needle jabs. Oh, and one session of glue torture.
It had been a hell of a week.
Epilogue
Some fun numbers to round out the story:
- Total number of hospitals involved: 2
- Total number of IV lines: 3
- Total number of hospital rooms: 3
- Total number of nurses I can recall: 19
- Total number of doctors I can recall: 7
- Total number of tests: 50
- Number of tests involving needles: 39
- Hospital 1 – Final cost before insurance: $15,726.64
- Hospital 2 – Final cost before insurance: $63,082.85
- ICU: $38,250
- Non-private room: $8,453.00
- Lab Tests: $7,087.00
- Radiology: $1,126.00
- PT: $1,408.00
- Cardiology: $3,660.00
- Other Diagnostic: $1,726.00
- Pharmacy: $372.85
- Hospitals combined: Final cost before insurance: $80,501.49
- Total paid out of pocket: ~$2,000
Thank God for good insurance. [4]
One Week Later: I have a tendency to write such that the story can be somewhat entertaining, and while my family and I use humor to defuse stress, make no mistake that this entire ordeal was not any fun at all. While it no longer hurts to breathe, it was (and remained a week later) difficult to breathe. I am constantly out of breath, feel dim-witted in a way that I do not enjoy, move very slowly lest I get winded, and sometimes have to take a break and sit down halfway up a flight of stairs. Still, I used that infernal spirometer machine as much as I could.
Two Weeks later: I still have coughing fits, I wonder if I will ever be able to do things I love like cycling or even walking in the park, and generally feel like someone who had parts of their lungs die might feel. Every time I cough I wonder if I’ll throw a clot that will kill me. Spending even an hour doing something non-strenuous (like trying to write this) leaves me winded and tired, and I’ve had to take naps because I struggle to stay awake after even the slightest exertion – like talking on the phone. I can’t stand for more than a few minutes at a time without getting tired. While this should all improve over time, I don’t know if it will.
Three Weeks Later: I’d say that my bad:good days ratio is probably 3:1 which is better than it was, but still frustrating. I went to Starbucks to try and feel normal. I lasted 20 minutes and came home after which I passed out on the couch for three hours.
Four Weeks Later: (it’s taken me that long to write this, because even writing is exhausting). If I sit at my desk (with my leg elevated) I can go almost all day without coughing or getting winded. I can now climb the stairs without needing to rest but two flights wears me out. Taking a shower still leaves me winded, my leg still hurts if I don’t elevate it, and I still wonder if I’ll ever be normal again, but that’s starting to fade a bit. Weirdly, a week of forced immobility has helped my back tremendously. I even scheduled physical therapy.
And since this has so far been classified as idiopathic (without known cause), the fear of it happening again is ever present. I still have clots in my leg that my body is (presumably) slowly dissolving and absorbing, and from what I’ve read it could take months or even over a year for them to go away. My appointment with the hematologist is a month from now.
The minute I start to feel good and do something like write for a while or talk on the phone I spend the next hour feeling like I ran a 5k, which I suppose is better than a full marathon, neither of which I have ever actually done.
Total experience: 0/10 – Do not recommend
Postscript: My wife was a rock through all of this, as were my kids. I can’t imagine how scary it must have been for all of them. It’s one thing to be the one in the bed developing a healthy fear of needles, it’s quite another to be the loved ones watching it all happen while feeling utterly powerless as your whole life is turned upside down.
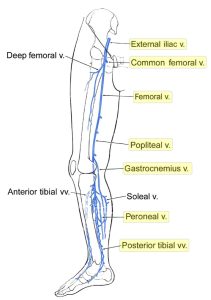 About three weeks into my recovery I was re-reading all the test results now that I could process things a bit better. The results of the ultrasound that I had in the ICU said:
About three weeks into my recovery I was re-reading all the test results now that I could process things a bit better. The results of the ultrasound that I had in the ICU said:
Acute extensive deep vein thrombosis of the right lower extremity with thrombus noted at the external iliac, common femoral, femoral, popliteal, gastrocenmius, posterior tibial and peroneal vein level.
No deep or superficial venous thrombosis of the left lower extremity.
To help visualize what all that means I looked up all the veins and found a picture of leg veins, then highlighted which of the veins in the pic had clots in them. As a friend said when I showed him the same picture, “That’s like, all the veins!” None of this was obvious to me until almost a month after the event.
It was bad — really bad — but I had zero clot load on my heart so hooray for missing out on the MOTHER OF ALL HEART ATTACKS.
Possible Root Cause: While trying to get my thoughts and memories in order to write this, a chain of events became clear to me, and I believe I have identified a potential root cause. This is more of what I’d call a disaster chain than a single event. In a nutshell:
 Feb 19: Steroid injection in right foot
Feb 19: Steroid injection in right foot- Feb 26: Oral steroids for back (6 days)
- Mar 4: Podiatrist commented on bruise at injection site
- Mar 13: Right leg swollen
- Mar 21: Woke up with chest pain
- Mar 23: went to ER, Admitted to ICU w/ DVT, PE, Pleural Effusion, and Infarcts
My theory is that a progression of unfortunate events all worked together to cause the DVT. Injections can (rarely) trigger DVT, though the information I’ve seen is usually related to intravenous drug users where the veins can be damaged. It is theoretically possible that the bruise on my foot was from nicking a vein in my foot during the injection, but I don’t believe this alone caused my DVT.
Steroid use can trigger DVT and PE, though the papers I’ve found all specify prolonged courses of corticosteroids. I’ve had many steroid injections in my life, all related to different joint problems, though they have usually been spread out by years if not decades. I had (if memory serves) three steroid shots in my foot over the past 24 months, which I can’t imagine was an issue, but coupled with the course of oral steroids (prednisone) which I charted as raising my blood pressure, I have to wonder if this tipped me over the edge when coupled with the bruising from the previous injection only 7 days prior.
Of course not going to the ER immediately upon noticing one swollen leg and then possibly biasing two healthcare professionals because I believed the swelling was due to overuse of Celebrex is completely on me.
Final Words (I Swear!)
Sorry for so many words (over 8,300!), but I felt the need to document this rather impactful event in my life. If it convinces even one person to go to the ER when one leg swells for no apparent reason, it will have been worth it. I’m glad I could be here to write it.
Thank you to the amazing teams at both hospitals, and thanks to my family for being there the entire time. Special thanks to Lauren for keeping me sane late at night when the Balrog tried to get me. She knows what it means.
Appendix – Footnotes
[1] My primary care provider is a nurse practitioner who is better than almost any doctor I’ve ever met, and I’ve met more than my fair share. My blood pressure was suddenly high and the cardiologist (who had an ego like every cardiac surgeon you may have seen on TV) gave me ALL the tests for a year and could not figure out the root cause so just said, “You have hypertension and will need to be on drugs for the rest of your life.” We literally had a screaming match when I told him he never gave me a root cause after which he yelled, and I quote, “Fine, stop taking the drugs then!” I walked out and told the front desk that I would never be back. My primary actually listened to me, had a hunch and sent me for a sleep study. A normal score is 5, I scored a 40, and within two weeks of starting with a CPAP machine my blood pressure was back to normal.
[2] It’s amazing what we can talk ourselves into. Even while writing and repeatedly editing this I’m amazed that I was so unconcerned about these events. My wife once told me that I was the dumbest smart person she had ever met. Apparently the proof just keeps rolling in on that one.
[3] I make a point of avoiding profanity on my sites because my mother (who’s been gone for over a decade now) wouldn’t approve, however if any situation warranted profanity, I feel like this one did.
[4] Any comments posted about the politics of the American healthcare system will be deleted.
Donate: PayPal Crypto:
ETH: 0x0AC57f8e0A49dc06Ed4f7926d169342ec4FCd461
Doge: DFWpLqMr6QF67t4wRzvTtNd8UDwjGTQBGs
Source of Nigel the Elephant’s name: https://www.youtube.com/watch?v=AiIlcew-GVM
This is all because of the politics of the US healthcare system. Who’s with me!
[GAD] This comment was left by my daughter and the only reasons I didn’t just delete it was a) because it really shows the depths of the snarky sarcastic humor we all share, and b) because she threatened to start a blog of her own called GAD.net supports CENSORSHIP!
Any and all other similar comments will be deleted without comment, clearly proving that I’m a fascist admin on a power trip.
Hello there Gary,
Please forgive the informality, but I almost feel as if I know you and the other regular contributors to Let’s Talk Guild, having been a daily reader for many years. As an aside, I live in Alverstoke, U.K and own a beautiful natural 2001 X500T, and a fiesta red (2000?) X160 Rockabilly.
I read the account of your recent awful experience with ever-opening eyes. I can absolutely empathise, although my tale of woe wasn’t anywhere as serious.
I’m a little older than you (just turned 66), retired, like guitars, walking, cycling and palaeontology. Crikey, this reads like a dating App!
Anyway, about this time last year, I had what I thought was the mother of all colds/coughs. All the normal symptoms and lasted about 3 weeks. I was too breathless to maintain my daily bike ride, and walking caused a pain in my ribs. Warning #1 ignored. Rationalised by “I must’ve pulled something coughing”. Things settled down for a couple of weeks, still breathless going up the stairs, but hey I’m 65 and haven’t done much exercise in a month. (Warning #2 ignored). A week or two later I figured I’d try a gentle bike ride, just 5 or 6 miles, to see how I coped physically. I managed about 3 miles before I had an excruciating pain in my back and had to walk home. (Warning #3 ignored). Rationalised by “well, it’s been a while, should’ve done a few stretches”). A few weeks later the cough returned. (Warning #4 ignored). Rationalised by “I can’t believe I’ve got another cold”. And then a few steaks of blood started to appear in the phlegm (terrible word, sorry). And you know what Gary, I was even then, even THEN, trying to rationalise it in my mind. “Well, I probably tore my throat with all this coughing, I’ll give it a week.” What was that you said, something to the effect of smart but dumb!
Anyway, I finally gave myself a figurative kick up the arse, contacted my General Practitioner, who if it wasn’t by phone, would’ve actually kicked me up the arse – happy, he was not!
I guess what followed was fairly standard. Same day chest X-RAY, “hmmm, something not quite right in your right lung, probably nothing, take antibiotics and have another X-Ray in a month”. The results of that second X-Ray resulted in a somewhat frantic trip to a different hospital for a troublesome day of CT and ultrasound scans.
I had made the mistake of accessing my patient records, and it seemed lung cancer was suspected, so when all the scan results were examined and they showed blood clots in the inferior vena cava and 2 pulmonary embolisms of the right lung, it was almost something to celebrate!
Re-reading the above, in retrospect, I can’t believe I was so stupid for so long.
Treatment started last September with daily blood thinners, probably for the rest of my life, as like you, the cause was idiopathic.
Anyway, like I said at the start, my experience was obviously nowhere near yours in terms of severity, but I thought you’d like to know that a fellow Guild nut shared a similar recent experience, and is now back to walking and breathing normally, and gradually building up the cycling mileage.
So hang in there Gary, things will improve. Your bike and the countryside are waiting, and summer’s just around the corner…
Ian.
That is quite the harrowing tale! Glad you’re OK and thanks for letting me know I’m not the only one who missed all the signs.